7 Interesting Facts About Diabetes
In 2021, an estimated 537 million adults were living with diabetes worldwide — roughly one in ten adults, according to the International Diabetes Federation. That scale matters: it drives healthcare planning, daily self-care needs, and the economic burden on families and systems.
These seven facts about diabetes are concise, evidence-backed and chosen to help you spot risk early, understand modern treatments and technologies, and separate useful guidance from common myths — with practical next steps you can use or share.
Medical and clinical insights
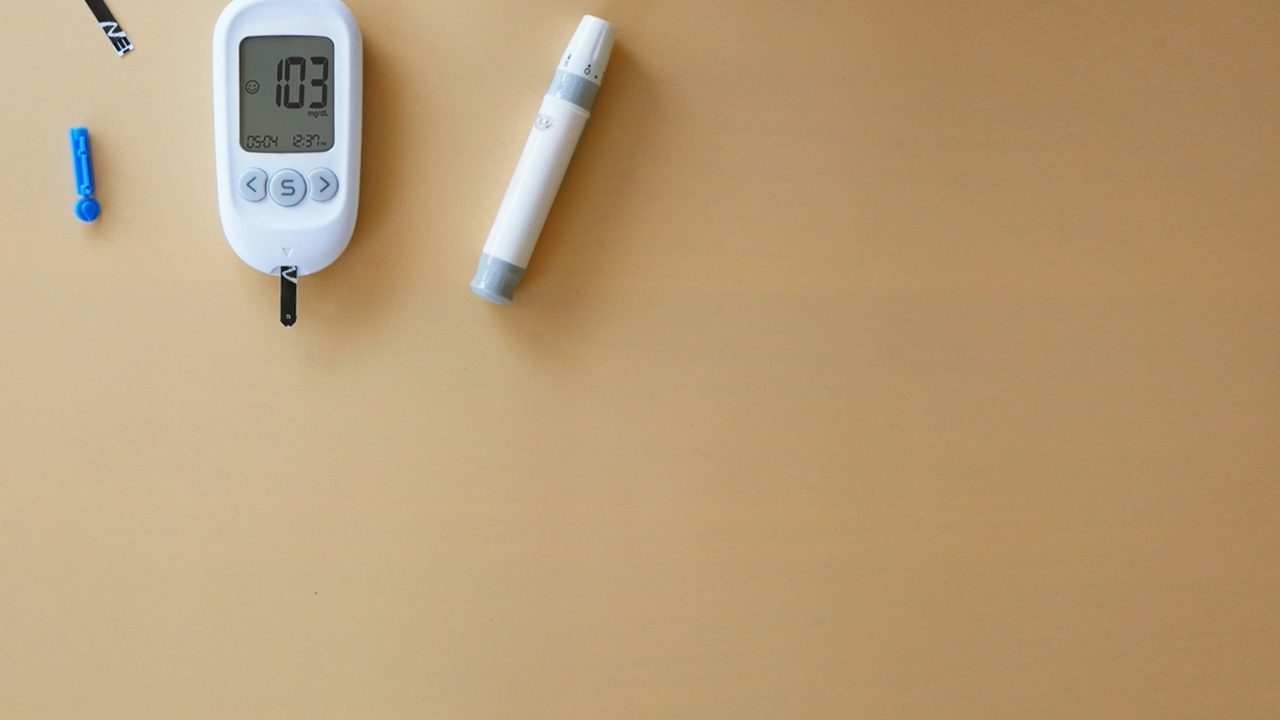
Clinical knowledge about diabetes has evolved dramatically since insulin was first used in humans after Banting and Best’s discovery in 1921. Today clinicians classify diabetes into several main types, screen for early disease, and tailor treatments to reduce long-term harm.
1. Global prevalence and the main types of diabetes
Diabetes affects more than half a billion adults worldwide: the IDF estimated 537 million in 2021, about one in ten adults. The three common clinical categories are type 1 (autoimmune, often starting in childhood and requiring insulin at diagnosis), type 2 (metabolic, strongly associated with age, adiposity and lifestyle), and gestational diabetes (glucose intolerance first identified during pregnancy).
High prevalence shapes screening and public-health planning: primary care teams often use risk scores and routine HbA1c or fasting glucose checks to find undiagnosed cases, and policymakers allocate resources for prevention, medications and complications care accordingly.
2. Early detection reduces the risk of serious complications
Earlier diagnosis and tighter glycemic control lower the chance of microvascular complications. Landmark work such as the UK Prospective Diabetes Study (UKPDS) showed that intensive glucose control reduced microvascular endpoints by roughly a quarter in people with newly diagnosed type 2 diabetes.
Practical screening includes periodic HbA1c tests, retinal exams and foot checks; the American Diabetes Association recommends screening adults with risk factors and using these routine checks to catch problems early and refer to eye, foot or kidney care when needed.
3. Medication advances (from insulin to GLP‑1s and SGLT2s) have changed outcomes
Treatment has come a long way since insulin’s discovery in 1921: modern rapid‑ and long‑acting insulin analogs make dosing more physiological, and two newer drug classes offer benefits beyond glucose lowering.
GLP‑1 receptor agonists (for example, semaglutide) help reduce weight and lower cardiovascular risk in several trials, while SGLT2 inhibitors (for example, empagliflozin) have shown cardiovascular and renal protection in major outcome trials like EMPA‑REG. Clinicians now individualize therapy to balance blood sugar goals, weight effects and organ protection.
Daily management and lifestyle
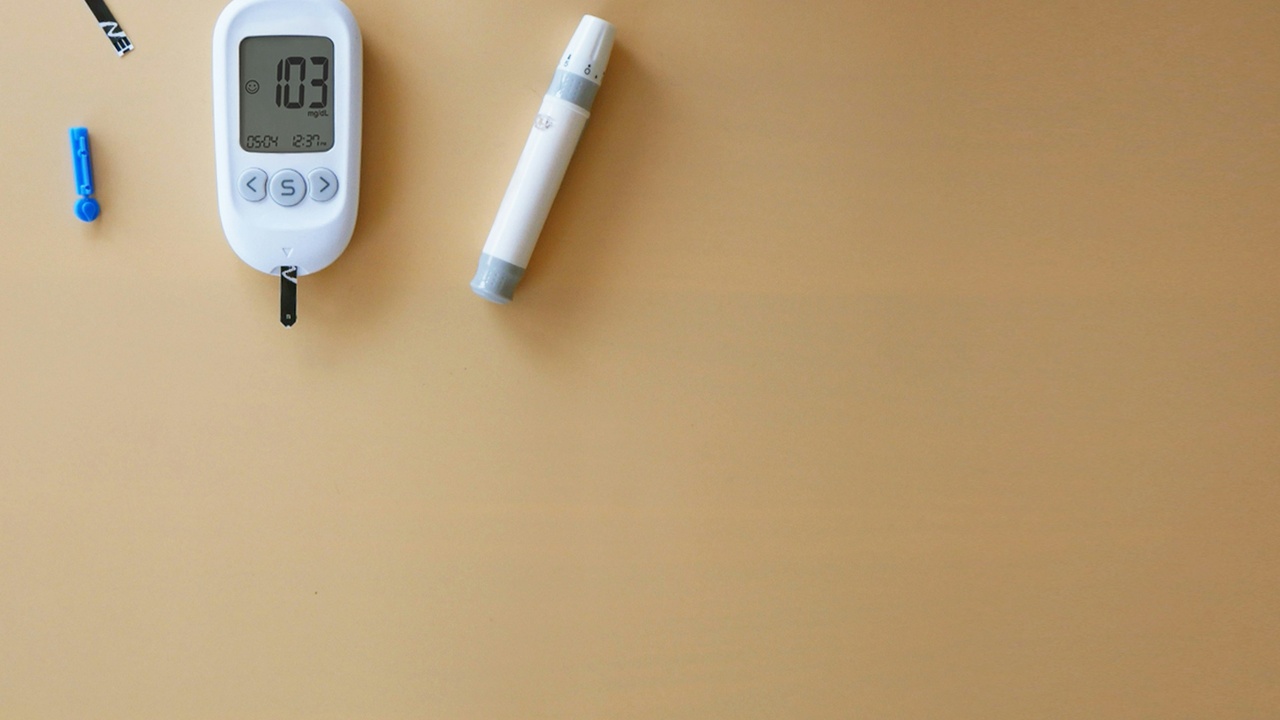
Small daily actions and affordable tools often produce outsized benefits for blood sugar and quality of life. Self-monitoring, structured lifestyle programs and clear, achievable targets help people delay or prevent type 2 diabetes and manage established disease more effectively.
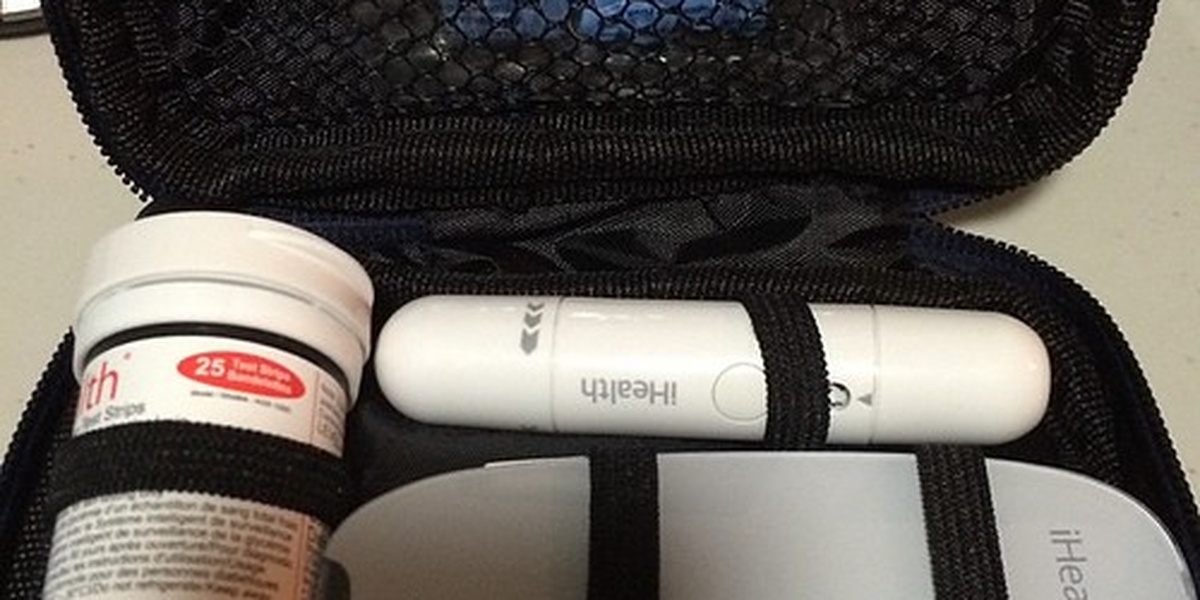
4. Self-monitoring — meters and continuous glucose monitors empower daily choices
Monitoring blood glucose gives immediate feedback that informs meals, activity and medication adjustments. Continuous glucose monitors (CGMs) such as Dexcom G6 and Abbott FreeStyle Libre provide trend data and alarms; trials and real‑world studies report improved time‑in‑range and fewer hypoglycemia events for many users.
For example, the FDA approved Dexcom G6 for adults in 2018, and users commonly use trend arrows to tweak a snack or delay insulin dosing when levels are rising. Clinicians still track A1c, but CGM metrics like time‑in‑range add useful day-to-day context.
5. Lifestyle changes can prevent or delay type 2 diabetes
Structured lifestyle programs can substantially reduce progression from prediabetes to type 2 diabetes. The Diabetes Prevention Program (DPP) demonstrated about a 58% reduction in diabetes incidence with an intensive lifestyle intervention over roughly three years, compared with placebo.
That intervention emphasized modest, achievable targets: 5–7% weight loss and about 150 minutes per week of moderate physical activity. The CDC now supports the National Diabetes Prevention Program, which adapts the DPP model for community and employer settings.
Social, economic, and technological impacts
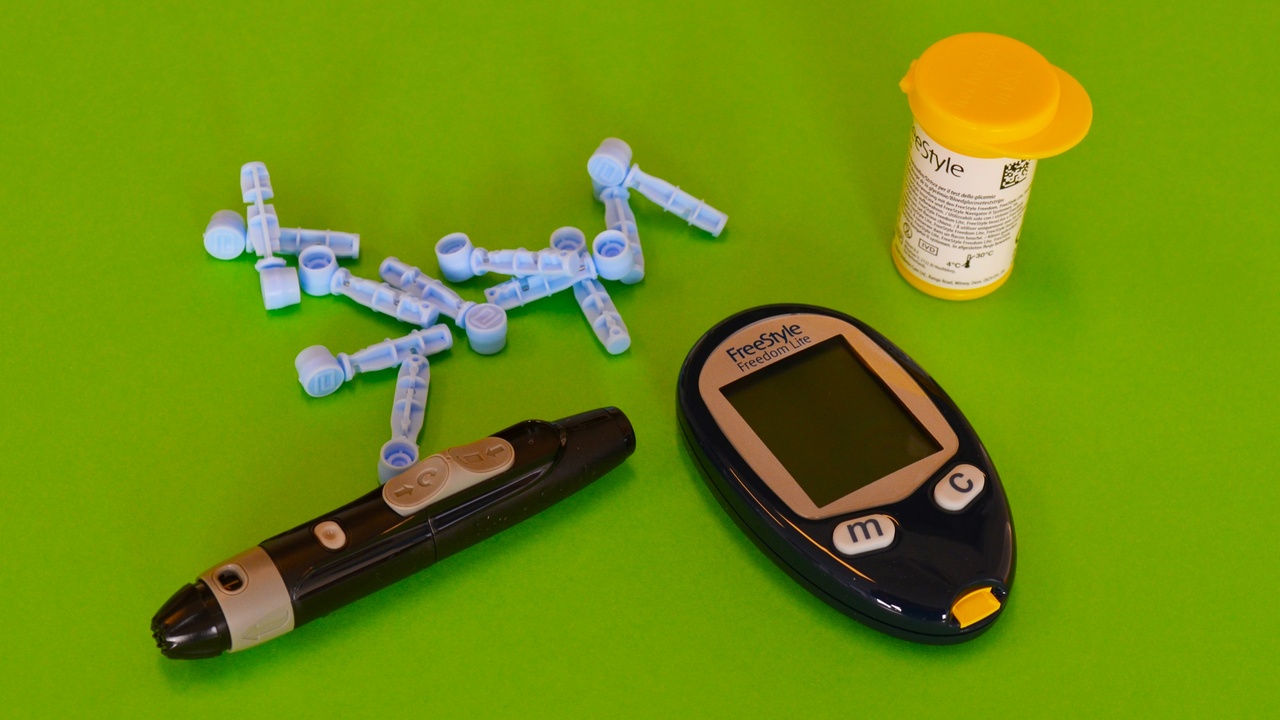
Diabetes affects societies far beyond clinical visits: it creates large direct medical costs, reduces productivity, and raises questions about access to affordable medications and devices. Policy, education and technology choices shape who benefits from advances.
6. Diabetes carries a substantial economic burden — but prevention and early care can be cost-effective
Global health expenditure on diabetes reached roughly USD 966 billion in 2021, per the IDF, and national figures are large as well — the U.S. estimated the total cost of diagnosed diabetes at about USD 327 billion in 2017 according to the CDC.
Costs come from hospitalizations, complications, medications and lost productivity. Investing in prevention programs (such as covered DPP offerings) and early treatment of complications often proves cost‑effective by avoiding expensive downstream care.
7. Clear public education and myth-busting improve outcomes and reduce stigma
Misconceptions persist — for example, saying sugar alone causes diabetes oversimplifies a multifactorial condition. Accurate public education encourages earlier screening, reduces shame and improves support for people who need treatment.
Organizations such as the American Diabetes Association and the CDC offer public resources, workplace guidance and school policies to accommodate students who need insulin or glucose monitoring. Community screening events and clear messaging can shorten delays to diagnosis and care.
Summary
- Diabetes is common — 537 million adults globally — and includes type 1, type 2 and gestational forms; screening helps find cases earlier.
- Early detection and control cut microvascular risk (UKPDS showed about a 25% reduction) and lower long‑term harm when paired with routine retinal, foot and A1c checks.
- Daily tools (CGMs, meters) and programs (DPP lifestyle intervention reduced incidence by ~58%) give practical ways to prevent or manage disease with targets like 150 minutes/week and 5–7% weight loss.
- Diabetes imposes large economic costs (global health spending near USD 966 billion in 2021); prevention, affordable access to insulin and devices, and clear education are high‑value priorities.
Check your risk factors, ask your clinician about appropriate screening or DPP programs, and if you or someone you know needs it, explore device and medication options (including CGMs and newer drug classes) while supporting policies that improve affordable access to essential therapies.