In 1928 Alexander Fleming noticed that a mold called Penicillium killed bacteria on a petri dish—an accidental discovery that launched the antibiotic era and saved millions of lives.
Yet despite that success, misunderstandings about these drugs persist and change how people use them, sometimes with dangerous results. Misuse fuels allergic reactions, Clostridioides difficile infections, and the spread of resistant bacteria that undermine modern medicine.
Antibiotic resistance already has measurable impact: a 2019 Lancet analysis estimated about 1.27 million deaths were directly attributable to bacterial antimicrobial resistance, and the CDC estimates roughly 30% of outpatient antibiotic prescriptions may be unnecessary.
Despite their life-saving role, antibiotics are surrounded by persistent myths that lead to misuse, harm patients, and drive antibiotic resistance; understanding and correcting these misconceptions is essential.
This article debunks seven common misunderstandings about antibiotics, shows the evidence behind good practice, points out practical signs to watch for, and suggests safer alternatives when appropriate.
When antibiotics actually help — and when they don’t

Antibiotics are designed to kill or inhibit bacteria; they do not act on viruses, which replicate inside human cells. That basic distinction explains why many common respiratory illnesses—colds, influenza, and many sore throats—won’t respond to antibiotics.
Clinicians use symptoms plus tests to decide. Rapid antigen tests for strep throat, urine dipsticks and cultures for urinary tract infections, and chest X-rays or clinical scoring for pneumonia often guide treatment decisions (a practice rooted in the post‑Fleming era of targeted therapy).
When in doubt, watchful waiting is reasonable in many outpatient cases: symptomatic care, hydration, rest, and follow-up instructions reduce unnecessary antibiotic exposure without increasing risk for uncomplicated viral illnesses. Ask your clinician whether testing or watchful waiting is appropriate for your symptoms.
Practical reader action: next time you’re prescribed an antibiotic, ask whether the infection is likely bacterial and whether a rapid test or observation period is a safe option.
1. Myth: Antibiotics treat viral infections (colds, flu, COVID-19)
This claim is false. Antibiotics target bacterial processes—cell wall synthesis, protein production, DNA replication—whereas viruses hijack host cells to replicate, so antibiotics have no direct effect on them.
CDC guidance is clear: antibiotics do not work for viral infections. Still, roughly 20–40% of outpatient antibiotic prescriptions are for conditions where they provide no benefit, driven by diagnostic uncertainty and patient expectations (CDC estimates ~30% unnecessary prescriptions).
Alternatives include symptomatic treatment (decongestants, pain relievers, saline rinses) and antivirals when indicated—oseltamivir for influenza started within 48 hours, or nirmatrelvir/ritonavir for high‑risk early COVID-19 in eligible patients.
2. Myth: A sore throat always needs antibiotics — better safe than sorry
Most sore throats are viral. Streptococcal pharyngitis (strep throat) is the main bacterial cause that benefits from antibiotics, but its prevalence differs by age—about 5–15% of adults and roughly 20–30% of children with sore throat have strep.
Clinicians often use the Centor score (fever, absence of cough, swollen anterior cervical nodes, tonsillar exudates) plus rapid antigen detection tests to decide who should get antibiotics. A rapid strep test in clinic gives fast, actionable results.
Unnecessary antibiotics expose patients to side effects and select for resistance. Seek testing or treatment if you have high fever, tender neck nodes, or no cough; otherwise, symptomatic care and follow‑up are usually safe.
3. Myth: Antibiotics speed recovery for most respiratory infections
For many respiratory conditions—acute bronchitis and most uncomplicated sinusitis—antibiotics show minimal benefit and symptoms often improve in days without them. Landmark trials and guidelines (including IDSA guidance for sinusitis) support conservative management in many cases.
Exceptions exist: bacterial pneumonia typically requires antibiotics, chosen based on patient age, comorbidity, and local resistance patterns (common outpatient options include doxycycline, amoxicillin‑clavulanate, or macrolides depending on context).
Actionable advice: try symptomatic relief and watchful waiting for uncomplicated bronchitis or mild sinusitis, and seek urgent care for red flags—high or persistent fever, shortness of breath, chest pain, or rapidly worsening symptoms.
How to use antibiotics responsibly: dose, duration, and access

Proper antibiotic use means the right drug at the right dose for the right duration, prescribed for a confirmed or strongly suspected bacterial infection. Dosing must match the drug’s pharmacology and the infection site; under‑dosing risks treatment failure and resistance, while excessive exposure raises adverse‑event risk.
Guidelines and stewardship programs increasingly support shorter courses for selected infections. For example, uncomplicated urinary tract infections and some community‑acquired pneumonias now have evidence supporting 3–5 day regimens in appropriate patients, rather than older 7–10 day defaults.
Never use leftover antibiotics or someone else’s prescription. If you have leftover pills, dispose of them through a pharmacy take‑back program or household hazardous waste collection. When in doubt, consult your clinician or pharmacist rather than self‑treat.
Hospitals and health systems (NHS, CDC stewardship initiatives) run antibiotic stewardship programs that tailor duration and choice of agents to the best available evidence, reducing harms while preserving effectiveness.
4. Myth: You must always finish a long course of antibiotics — stop early if you feel better
Advice to “always finish the course” was widespread, but guidance is evolving. The traditional rationale—that stopping early fosters resistance—was based on older concepts, and recent trials show shorter courses can be equally effective for certain infections while reducing side effects.
Examples: uncomplicated urinary tract infections often respond to 3–5 day regimens, and some community‑acquired pneumonia trials support shorter courses when clinical improvement is rapid. However, any change to duration should come from your clinician—don’t stop or shorten therapy on your own.
If you experience adverse effects, contact your prescriber promptly; they may switch agents or adjust the plan rather than leaving you untreated or risking harm.
5. Myth: It’s okay to keep leftover antibiotics or share prescriptions
Keeping or sharing leftovers is risky. The drug may be inappropriate for the new illness, the dose might be wrong, and allergies or contraindications could cause serious harm. Sharing masks the need for proper diagnosis and contributes to resistance.
Some antibiotic classes have specific safety concerns: fluoroquinolones carry tendon‑rupture and nerve injury warnings, and tetracyclines are contraindicated in pregnancy and young children due to tooth and bone effects.
Dispose of leftovers at pharmacy take‑backs or community collection points. If you think you need treatment, see a clinician or pharmacist rather than using someone else’s prescription.
Safety, side effects, and the broader problem of resistance
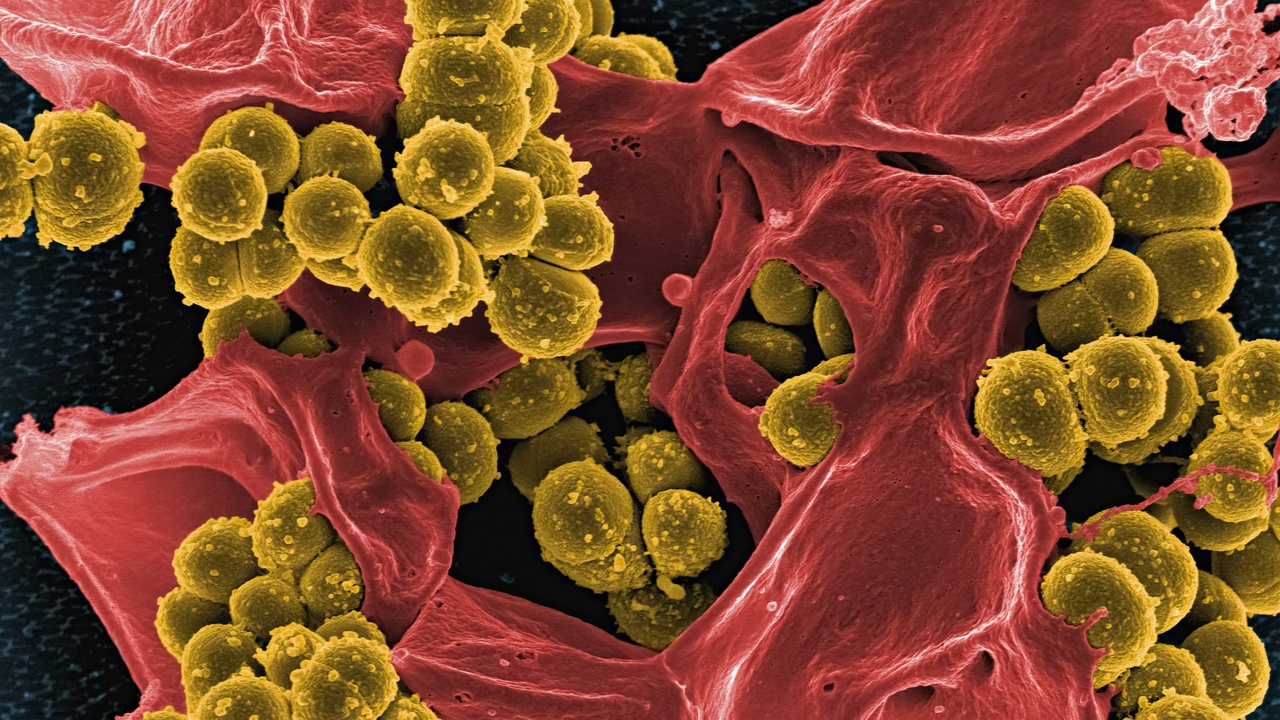
Antibiotics save lives, but they also carry risks: mild effects like gastrointestinal upset and yeast infections, severe allergic reactions such as anaphylaxis, and C. difficile colitis which can cause hospitalization and death. At the population level, misuse selects for resistant organisms that spread in communities and healthcare settings.
Global data are sobering. The 2019 Lancet study estimated roughly 1.27 million deaths were directly attributable to drug‑resistant bacterial infections, and earlier projections (the 2016 O’Neill report) warned resistance could cause up to 10 million deaths annually by 2050 without action.
Individual choices matter: vaccination reduces infections that might otherwise prompt antibiotic use; hand hygiene and safe food handling limit transmission; and avoiding unnecessary antibiotics helps preserve effectiveness for everyone.
Talk with your clinician about stewardship: ask whether an antibiotic is truly needed, whether a narrow‑spectrum agent or shorter course is appropriate, and how to recognize and report adverse effects.
6. Myth: Antibiotics are harmless — side effects are rare and mild
Antibiotics are not harmless. Common adverse effects include nausea, diarrhea, and yeast infections, but serious harms occur: C. difficile infections cause tens of thousands of deaths annually in the U.S., and true penicillin anaphylaxis—though uncommon (roughly 0.01–0.05% of exposures)—can be life‑threatening.
Other drugs have notable risk profiles: fluoroquinolones have associations with tendon injury and peripheral neuropathy, and some agents require dose adjustment for renal impairment. Keep an up‑to‑date allergy history and report suspected adverse reactions to your provider or national reporting systems.
7. Myth: Antibiotic resistance is someone else’s problem — hospitals will handle it
Resistance is a community and global issue. Resistant strains like MRSA now circulate outside hospitals, and outpatient antibiotic misuse contributes to that spread. The Lancet’s 2019 figures show the global mortality burden is already real and uneven across regions.
Resistance also has economic costs: lost productivity, longer hospital stays, and more expensive therapies. Public‑health measures—vaccination programs, infection control, and stewardship—reduce this burden, but they require widespread participation.
Practical steps you can take: stay up to date on vaccines, practice hand hygiene, avoid pressuring clinicians for antibiotics, and support local stewardship efforts through your healthcare contacts and community advocacy.
Summary
- Antibiotics only treat bacterial infections; many common respiratory illnesses are viral and don’t benefit from antibiotics.
- Misuse causes real harms: side effects (including C. difficile and allergic reactions) and the spread of resistant bacteria that contributed to about 1.27 million deaths in 2019.
- Clinical testing (rapid strep, urine tests, imaging) and stewardship programs help tailor drug choice and duration; shorter courses are appropriate for some infections when guided by evidence.
- Individual actions matter: ask about testing or watchful waiting, never share or keep leftovers, get vaccinated, and practice good hygiene to protect yourself and the community.