In 1796 Edward Jenner took pus from a cowpox sore and used it to protect a young boy against smallpox — an experiment that planted the seed for modern vaccination. A long, concerted global effort followed: the World Health Organization launched its smallpox eradication program in 1967, and smallpox was officially declared eradicated in 1980.
That long arc, from Jenner’s benchwork to the last naturally occurring case, helps explain why vaccines remain central to public health. Vaccines are one of public health’s most powerful and evidence-backed tools — they prevent disease, save lives, reduce costs, and continue to evolve with new science. Below you’ll find ten clear, sometimes surprising facts about vaccines that span history, science, society, and the future.
Historical and Public Health Impact
Vaccines reshaped patterns of human disease within decades. Early experiments like Jenner’s cowpox inoculation introduced the basic idea: expose the immune system safely so it remembers a pathogen without causing the full illness.
In the 20th century, organized campaigns scaled those ideas. The World Health Organization ran a global smallpox campaign starting in 1967 that used mass vaccination and ring-vaccination strategies; by 1980 smallpox no longer occurred naturally anywhere. Other campaigns cut diphtheria and tetanus deaths and reduced childhood scourges through routine immunization.
These programs produced measurable drops in disease incidence and freed up health resources for other priorities, from maternal care to chronic disease management.
1. Smallpox was eliminated — a first for a human disease
Smallpox is the only human disease eradicated globally. The World Health Organization launched its coordinated eradication effort in 1967, and after intensive vaccination and surveillance the disease was declared eradicated in 1980.
That outcome meant no more natural cases, routine smallpox vaccination was stopped in many places, and public-health resources could be reallocated to other needs. The campaign’s use of ring vaccination — immunizing close contacts around detected cases — proved decisive.
2. Vaccination cut childhood deaths by the millions
Routine vaccines prevent roughly 2–3 million deaths each year worldwide, according to World Health Organization estimates. Vaccination against measles, diphtheria, pertussis and Haemophilus influenzae type b drove large early declines in childhood mortality.
For example, measles deaths have fallen by more than 70% since 2000 as coverage expanded, translating to far fewer hospitalizations and lifelong disabilities such as vision loss or brain injury from severe infection.
3. Polio is nearly gone thanks to sustained vaccination
The Global Polio Eradication Initiative began in 1988, and wild poliovirus cases have declined by over 99% since then. Only a handful of endemic areas remain, and persistent, targeted campaigns are required to finish eradication.
Different tools helped in different phases: oral live-attenuated vaccines interrupted transmission in communities, while inactivated vaccines have been used to eliminate vaccine-derived risks as regions move toward eradication.
How Vaccines Work and Medical Benefits
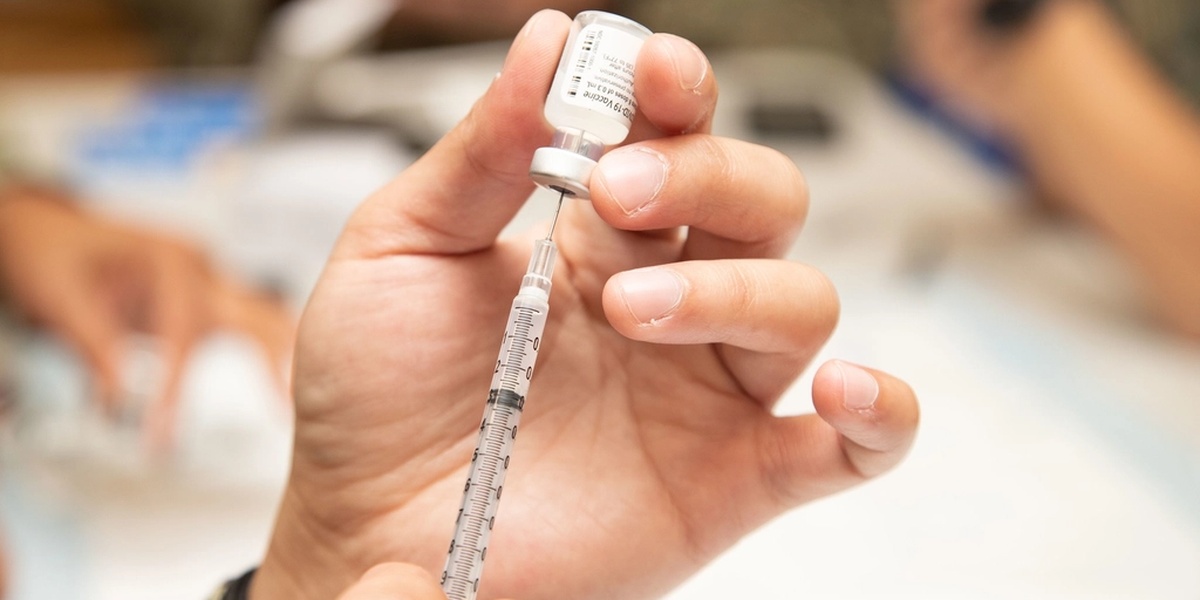
Vaccines teach the immune system to recognize specific antigens so it can respond faster and stronger on real exposure. They mimic infection without causing disease, prompting memory B and T cell formation that limits future illness and complications.
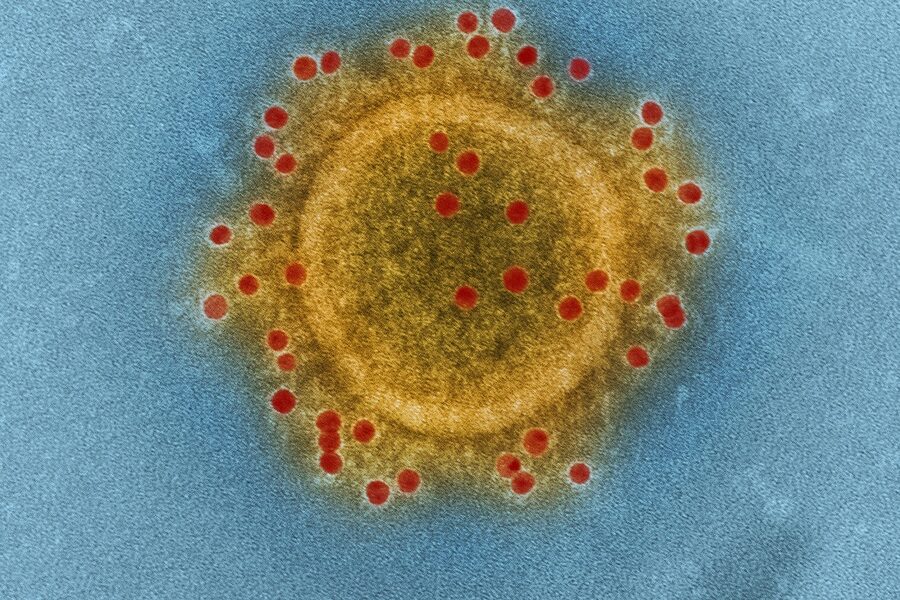
Multiple platforms exist: live-attenuated, inactivated, subunit, viral-vector and mRNA vaccines each present antigens in different ways. Recent examples include mRNA vaccines for COVID-19 (Pfizer-BioNTech, Moderna) and traditional inactivated influenza shots.
4. Vaccines train the immune system without causing the disease
That training is the central benefit: vaccines create durable immune memory so exposure later produces little or no illness. Live-attenuated vaccines (like measles) use weakened pathogens, while inactivated vaccines present killed organisms or purified components.
Newer platforms proved their worth during COVID-19: mRNA vaccines received emergency use authorization in December 2020 and showed initial efficacy of roughly 94–95% in clinical trials for preventing symptomatic disease, greatly reducing severe outcomes and hospitalizations.
5. Herd immunity protects people who can’t be vaccinated
When enough people are immune, a pathogen struggles to spread. Herd-immunity thresholds vary by disease; measles requires about 95% coverage to stop sustained transmission.
High coverage therefore protects infants who are too young for certain shots, people with immunosuppression, and those allergic to vaccine components by reducing the chance they encounter the pathogen.
6. Vaccines prevent long-term complications, including cancer
Vaccination can avert chronic consequences that appear years later. The HPV vaccine, first licensed in 2006 (Gardasil), prevents infections that cause cervical and other cancers, and countries with high coverage have seen large drops in vaccine-type HPV infections and precancerous lesions.
Hepatitis B vaccination, given routinely to infants in many countries, prevents chronic hepatitis and substantially reduces the risk of liver cancer decades after infection would have occurred.
Societal and Economic Benefits
Beyond health, vaccines deliver strong economic returns: they reduce medical spending, prevent productivity losses, and help keep schools and workplaces open.
For communities, fewer outbreaks mean steadier services, less strain on hospitals, and lower costs for long-term care. During large vaccination campaigns, governments often see measurable budgetary and social benefits.
7. Vaccines save healthcare dollars — often billions
Economic analyses show vaccination programs generate huge savings. For U.S. birth cohorts from 1994–2013, the CDC estimated routine childhood vaccination prevented roughly 322 million illnesses and saved about $295 billion in direct costs and roughly $1.38 trillion in societal costs.
Those savings come from fewer hospitalizations, less need for long-term disability care, and avoided outbreak responses that can be very expensive at scale.
8. Vaccines keep schools and economies running
High vaccination coverage reduces severe disease and hospital load, which supports phased reopenings and sustained economic activity. Early COVID-19 vaccine rollouts in 2021 correlated with sharp declines in hospitalization among vaccinated groups, often around 80–90% effectiveness against severe outcomes.
That drop in severe cases translated to fewer missed school days, steadier workforce attendance, and less pressure on healthcare systems during waves of infection.
Innovation, Safety and the Future of Vaccines
Recent innovations — mRNA, viral vectors, new adjuvants — shorten development timelines and expand what’s possible. At the same time, safety systems operate continuously to detect and investigate rare adverse events after rollout.
These advances mean researchers can pursue tougher targets and update vaccines more quickly when pathogens change, while regulators and surveillance networks maintain careful oversight.
9. New platforms mean faster vaccine development
Platform technologies dramatically shortened timelines during the COVID-19 pandemic: the virus was identified in early 2020 and vaccines reached emergency use authorization around December 2020 — roughly a 12‑month timeline from pathogen ID to public use.
Because mRNA and similar platforms reuse a common manufacturing approach, they can be adapted quickly for new pathogens or variants. Ongoing trials are testing mRNA vaccines for seasonal influenza and even personalized cancer vaccines.
10. Vaccine safety monitoring is rigorous and continuous
Vaccines undergo multiple trial phases before authorization and are monitored afterward by systems like VAERS and the Vaccine Safety Datalink in the U.S., and by EMA and WHO pharmacovigilance internationally.
These systems detect rare signals and prompt formal investigations; serious allergic reactions for many vaccines occur on the order of about 1–5 per million doses. Regulators then review data and update guidance to protect the public.
Summary
- Smallpox eradication (declared 1980) shows vaccines can eliminate diseases through coordinated global effort.
- Vaccination prevents roughly 2–3 million deaths each year and dramatically reduces childhood illness and long-term disabilities.
- Platform advances like mRNA enabled vaccines to reach the public within about a year in 2020–2021, speeding responses to new threats.
- Strong safety monitoring continues after approval; serious adverse events are very rare (about 1–5 per million for many vaccines).
- These facts about vaccines point to both historic achievements and future opportunities — check your national immunization schedule or consult trusted sources such as the World Health Organization or the CDC for guidance.