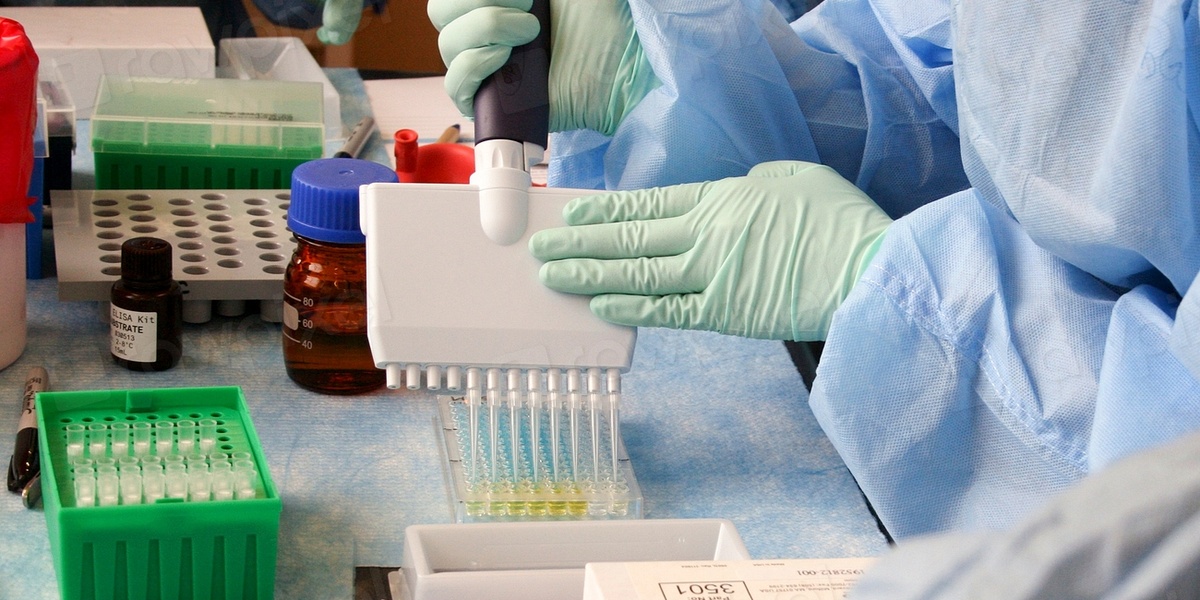
The story of modern diagnosis begins with a microscope and a stubborn idea. In the mid‑1800s, advances in microscopy and acceptance of germ theory transformed medicine: diseases once diagnosed by symptoms alone began to be identified by organisms and chemical signals invisible to the naked eye. By the late 1800s hospitals started to build small testing labs; over decades those benches became clinical diagnostic centers that shape nearly every treatment decision today. The distinction between two commonly used labels — clinical laboratory science and medical laboratory science — matters for students choosing a program, managers hiring staff, and clinicians who rely on lab expertise. While the terms clinical laboratory science and medical laboratory science are often used interchangeably, they reflect meaningful differences in education, certification, workplace roles, scope of practice, and regulatory context — differences that matter for students, hiring managers, and clinicians.
Education & Certification Differences
1. Program names and degree requirements differ
Some universities call their four‑year program Medical Laboratory Science (MLS); others label it Clinical Laboratory Science (CLS). That naming often signals whether the curriculum emphasizes clinical reasoning, management, or bench skills, but both can prepare graduates for similar clinical roles when NAACLS accreditation is in place.
Typical lengths are clear: a BS in MLS/CLS is about four years, while Medical Laboratory Technician (MLT) or associate programs usually run two years. NAACLS accreditation remains the primary marker of program quality and alignment with entry‑level competencies.
The practical implication: employers often expect a bachelor’s graduate for high‑complexity testing or supervisory roles, while associate graduates fill technical bench positions and can progress later with additional training or degrees.
2. Certification pathways and credential names vary
Credential names map to different exams and eligibility rules. The ASCP Board of Certification (BOC) issues common credentials such as MLS(ASCP) and MLT(ASCP), each with distinct coursework and clinical practicum hour requirements.
As a concrete example, graduates of a NAACLS‑accredited bachelor’s program typically qualify to sit for the MLS(ASCP) exam, whereas graduates from a two‑year associate program pursue MLT(ASCP) certification. Some schools award a CLS degree title but the curriculum still meets MLS(ASCP) eligibility; regional naming varies.
Certification determines job eligibility in many hospitals, so the diploma title alone doesn’t guarantee the credential employers expect.
3. Continuing education, licensure and professional societies differ
After initial certification, maintenance rules diverge. Most ASCP credentials require periodic renewal and continuing education (CE) credits; renewal cycles commonly fall every two years for many credentials.
State licensure adds another layer. States such as California and New York have their own licensing or registration requirements that can exceed national certification rules. That affects mobility and hiring decisions.
Professional societies like ASCLS and ASCP provide CE, advocacy, and job resources. Employers often expect staff to meet CE quotas and to document competency for specialty testing.
Roles, Responsibilities & Work Settings
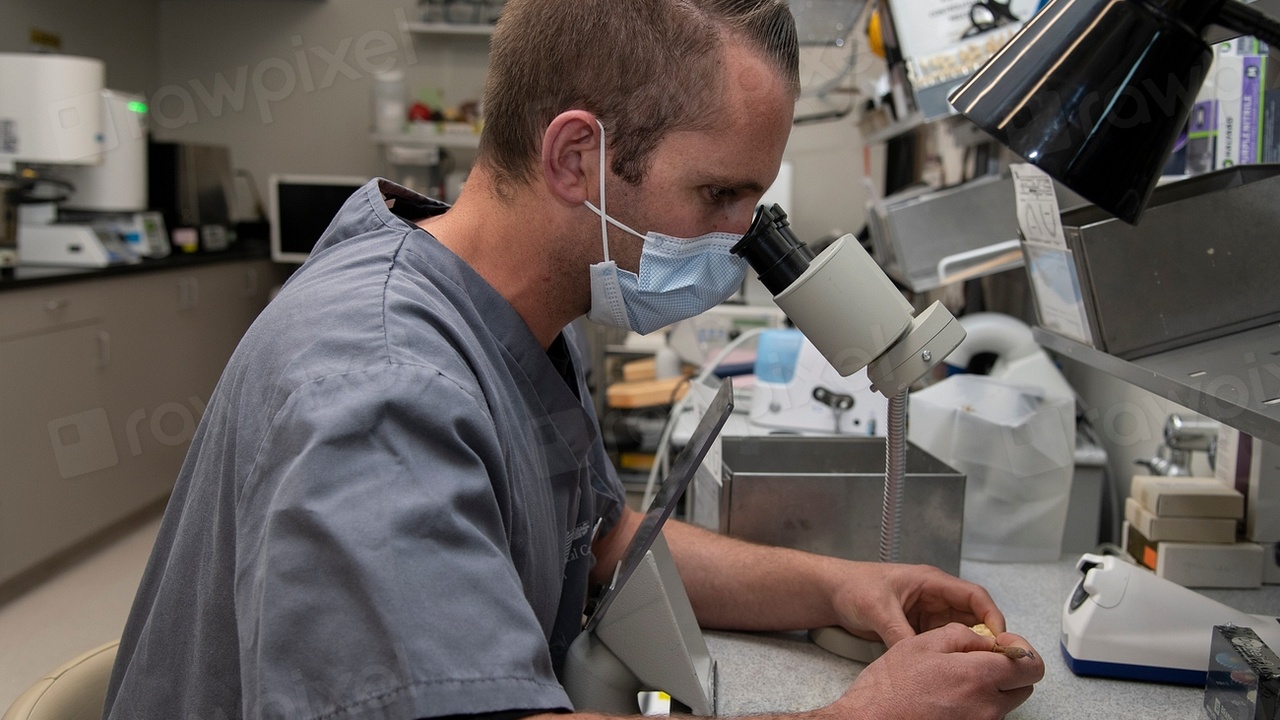
4. Clinical emphasis vs technical focus in daily duties
Day‑to‑day duties shift with setting. Hospital MLS/CLS roles often include clinical interpretation and direct consultation with physicians, while reference lab roles emphasize throughput, automation, and strict QC routines.
For example, a microbiologist in a hospital may discuss culture and susceptibility findings with an infectious disease team to guide antibiotic choice. Contrast that with a reference lab running thousands of PCR tests per week where the priority is consistent instrument performance and rapid turnaround.
Both require technical skill, but the soft skills and clinical judgment expected from MLS/CLS graduates tend to be greater in patient‑facing settings.
5. Typical workplaces and their expectations differ
Professionals work across hospitals, physician‑office labs, public health departments, academic research labs, biotech, and diagnostics companies. Each employer prioritizes different competencies.
Hospitals expect broad clinical knowledge, rapid troubleshooting, and availability for shift work; many hospital labs operate 24/7 with night and weekend shifts. Reference labs like Quest Diagnostics value instrument maintenance and sample logistics. Industry roles at firms such as Thermo Fisher or Roche emphasize assay validation and regulatory documentation.
Public health labs collaborate with the CDC on outbreak response and expect strong molecular and epidemiologic skills. Job titles alone don’t guarantee duties; read job descriptions closely.
6. Career advancement and specialization tracks vary
Common advancement follows bench scientist → lead technologist → supervisor/manager → director. Alternative tracks include education, research, sales, or regulatory affairs. Advanced degrees open academic and scientific leadership roles.
There are roughly six core specialty areas employers recognize: Microbiology, Hematology, Clinical Chemistry, Blood Bank (immunohematology), Molecular Diagnostics, and Immunology. Technologists often specialize in one or two areas, then expand into leadership or consulting roles.
An MLS may become a lab manager at a hospital, then move into clinical consulting for a diagnostics firm, illustrating how credential and experience shape career arcs.
Scope of Practice, Technology & Regulation
7. Regulatory distinctions and test complexity
CLIA, enacted in 1988, classifies tests into three complexity levels: waived, moderate, and high. Staffing and documented competency must align with the complexity of tests a lab performs.
High‑complexity testing typically requires personnel with a bachelor’s degree and documented training and competency. Many molecular PCR panels and multiplex infectious disease assays fall into the high‑complexity category and demand more rigorous oversight.
Regulatory classification affects hiring, training budgets, and who may sign out results. That’s why employers often list required credentials tied to CLIA responsibilities.
8. Technology, methods and clinical integration differ
Programs and job descriptions emphasize different blends of manual technique, automation, and data interpretation. Modern clinical labs use high‑throughput analyzers, multiplex PCR, next‑generation sequencing, and laboratory information systems.
Practical skills include instrument operation and maintenance, quality control, and result validation. Examples of common platforms include Roche Cobas and Abbott Architect for clinical chemistry, and Thermo Fisher QuantStudio for qPCR assays. Molecular diagnostics expanded through the 1990s and grew sharply in the 2000s, changing day‑to‑day lab duties.
As automation increases, the role of the MLS/CLS often shifts toward interpretation, troubleshooting, and ensuring clinical relevance of results rather than only performing manual tests.
Summary
- Naming can mask important program and credential differences; check NAACLS accreditation and ASCP eligibility when choosing or hiring a program graduate.
- Workplaces set expectations: hospitals favor clinical consultation and shift flexibility; reference labs emphasize automation and volume; industry requires validation and regulatory know‑how.
- Regulation ties staffing to test complexity — CLIA (1988) uses three categories (waived, moderate, high) and influences who may perform which assays.
- Before committing to a program or making a hire, confirm program accreditation (NAACLS), certification pathways (ASCP BOC), and any state licensure rules that apply.