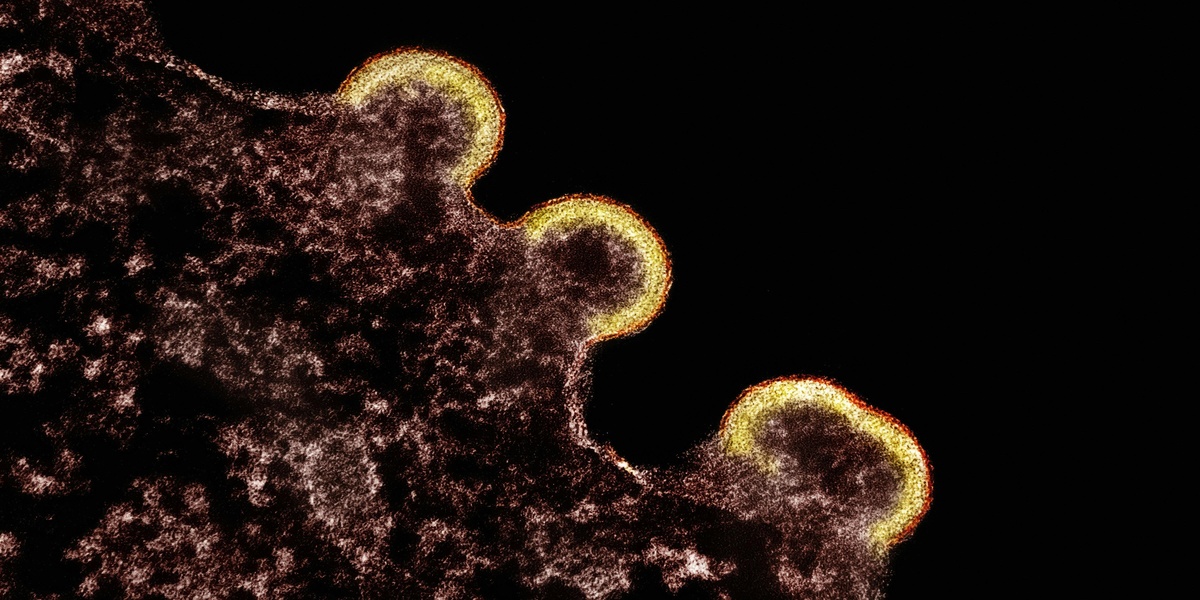
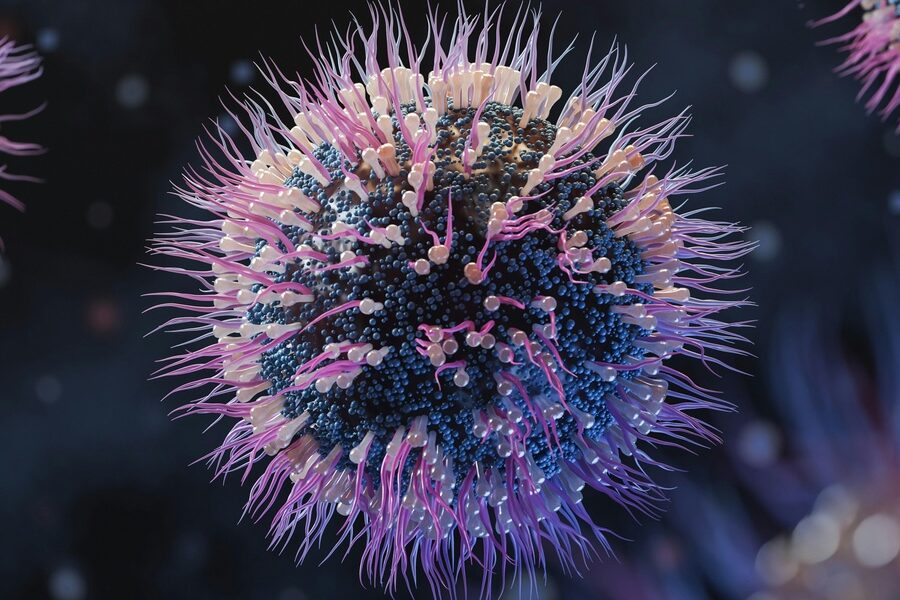
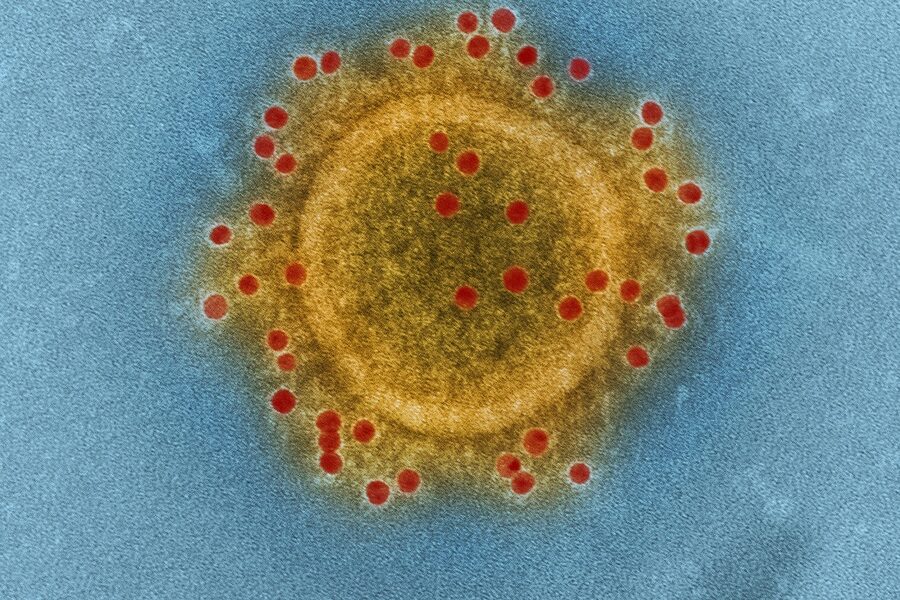
In the late 19th century Robert Koch and Louis Pasteur proved microbes cause disease, and just a few decades later scientists separated bacteria from an entirely different class of agents: viruses (Ivanovsky and Beijerinck, 1890s). That history helps explain why telling bacteria and viruses apart still matters in the clinic and at home.
For patients it changes treatment: antibiotics work on bacteria but not on viruses, so a correct diagnosis spares side effects and preserves future options. For clinicians it guides testing and stewardship; the CDC estimates at least 30% of outpatient antibiotic prescriptions are unnecessary. For policymakers the distinction shapes vaccination campaigns, outbreak response, and infection-control priorities.
Once I saw a young adult leave urgent care with a week’s worth of antibiotics for a clear viral cold—he felt better the next day from rest and fluids, not the pills. Practical differences like that add up. Below are eight evidence-backed differences between bacterial and viral infections, explained with examples and numbers clinicians and patients can use.
Clinical Presentation and Symptom Patterns
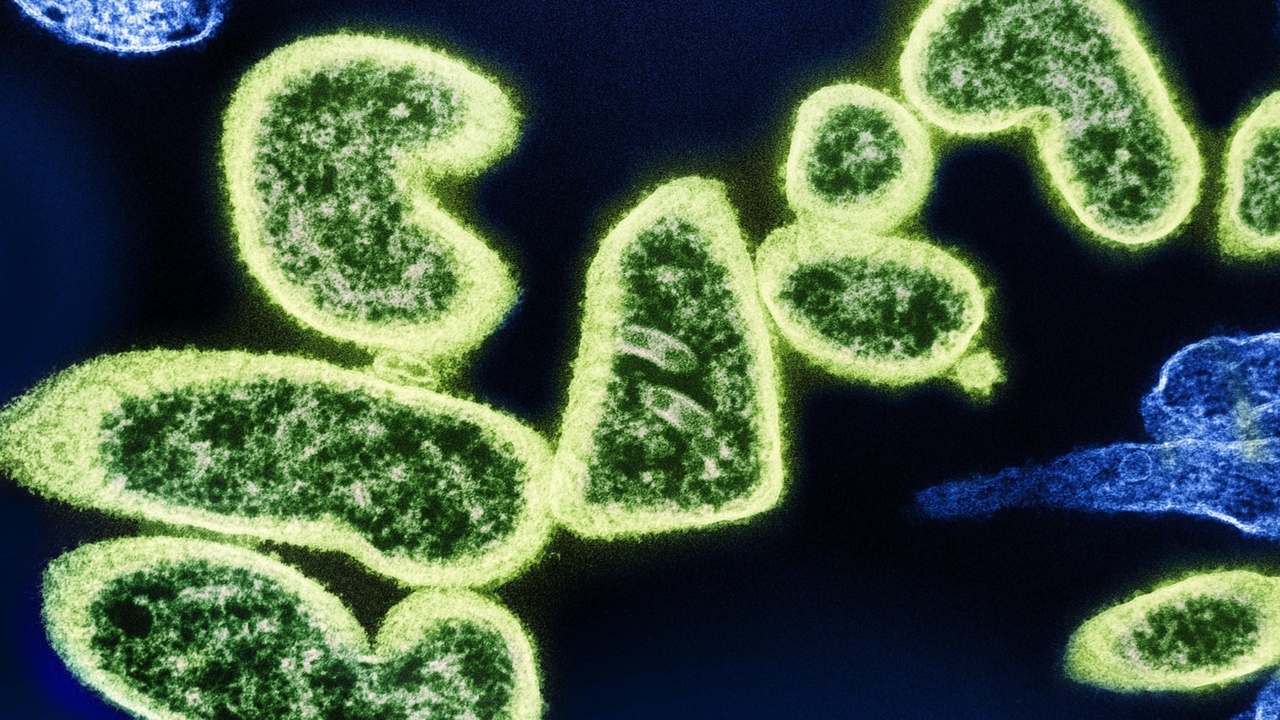
How an infection begins and how symptoms evolve often gives the first clue about whether microbes are bacterial or viral. While many exceptions exist, clinicians use timing, symptom distribution, and incubation periods as practical heuristics. For example, incubation ranges can help: streptococcal pharyngitis typically incubates 2–5 days, influenza 1–4 days, and SARS‑CoV‑2 from roughly 2–14 days. Those numeric ranges help triage in primary and urgent care, though testing is required for confirmation.
1. Onset and time course: bacterial infections often have localized, slower onsets while viral illnesses can be abrupt and systemic
Bacterial infections commonly present with a more focal onset over days, whereas many viral illnesses start abruptly with systemic symptoms like fever, body aches, and malaise. Incubation examples: Streptococcus pyogenes (strep throat) 2–5 days; influenza A 1–4 days; SARS‑CoV‑2 roughly 2–14 days.
In practice, that means a sore throat slowly progressing with localized tenderness and high-grade fever over 48–72 hours raises suspicion for strep, while sudden fever with myalgia and cough within 24–48 hours points to influenza. Triage decisions—testing, empiric antibiotics, or supportive care—use these patterns, but overlap exists and testing remains important.
2. Symptom patterns: localized purulence or focal pain often suggests bacteria; widespread respiratory or systemic symptoms suggest viruses
Rule of thumb: purulence, focal pain, and unilateral findings often indicate bacterial infection; diffuse congestion, sneezing, and bilateral symptoms usually reflect viral causes. For example, bacterial sinusitis is more likely when symptoms persist beyond 10 days with unilateral facial pain and purulent nasal discharge, while viral upper respiratory infections typically produce bilateral clear rhinorrhea and improve in 5–7 days.
Other examples: lobar consolidation on exam or chest x‑ray suggests bacterial pneumonia (Streptococcus pneumoniae), whereas viral bronchitis or bronchiolitis tends to cause diffuse wheeze and diffuse radiographic patterns. Symptom-based diagnosis can guide when to test or treat empirically, but clinicians should weigh severity, risk factors, and duration before starting antibiotics.
Cause, Structure and Transmission
Bacteria are single‑celled organisms with their own metabolism, while viruses are acellular particles composed of nucleic acid and protein that must hijack host machinery to replicate. Size gives a quick sense: bacteria are roughly 0.5–5 µm, visible under light microscopy; viruses range ~20–300 nm and require electron microscopy or molecular methods for detection. Structure affects how long agents survive outside the host and what control measures work best.
3. Agent biology: bacteria are cellular organisms; viruses are particles that hijack host cells
The core distinction is biological: bacteria carry metabolic pathways and can often grow on nutrient media, whereas viruses lack independent metabolism and need host cells to replicate. That difference explains why laboratories culture bacteria and why many viral diagnoses rely on nucleic‑acid detection.
Size matters clinically: bacteria such as Escherichia coli or Staphylococcus aureus (cellular organisms) are measured in micrometers; viruses like SARS‑CoV‑2 or influenza are measured in nanometers. Some bacteria—Chlamydia, Legionella—live inside cells and blur clinical presentations, but antibiotics remain effective against cellular organisms by targeting processes like cell‑wall synthesis.
4. Transmission and contagious period: environmental stability and transmission routes differ between many bacterial and viral pathogens
Transmission modes—droplet, airborne, contact, fecal‑oral—and environmental stability shape public‑health responses. Norovirus can persist on surfaces for days to weeks and is highly contagious, driving rapid outbreaks on cruise ships and in long‑term care; influenza viruses typically survive on surfaces for hours and spread mainly by droplets.
Examples: Mycobacterium tuberculosis transmits via airborne particles and, if untreated, patients can remain contagious for prolonged periods; measles (a virus) is extremely contagious by airborne spread but is largely preventable by vaccination. Understanding routes and survival helps set isolation duration, cleaning protocols, and contact‑tracing priorities.
Diagnosis and Laboratory Testing

Diagnostic approaches diverge because the agents differ. Bacteria are frequently identified by microscopy and culture with susceptibility testing, while viruses are most often detected by molecular methods (PCR) or rapid antigen assays. Turnaround time and test sensitivity trade off: cultures can take 24–72 hours (longer for slow growers), whereas PCR gives fast, sensitive answers useful for immediate infection‑control decisions.
5. Bacterial diagnosis: cultures, gram stain, and susceptibility testing guide targeted therapy
Bacterial diagnosis commonly uses gram stain and culture. Routine cultures grow organisms in 24–72 hours, after which labs perform identification and antibiotic susceptibility testing. These results let clinicians tailor therapy and practice stewardship rather than rely on broad empiric coverage.
Clinical examples include urine culture with colony counts confirming E. coli urinary tract infection or blood cultures identifying bacteremia in sepsis; Mycobacterium tuberculosis requires special media and may take weeks to grow. Susceptibility testing changes choices—switching empiric therapy to a narrow‑spectrum agent when appropriate reduces collateral damage.
6. Viral diagnosis: PCR and antigen tests prioritize speed and detection of nucleic acid
Many viral diagnoses depend on PCR (the sensitive gold standard) or rapid antigen tests that trade some sensitivity for speed. PCR results can be same‑day to 48+ hours depending on lab capacity; antigen tests give results in minutes and are useful for immediate isolation or cohorting decisions.
Examples: nasopharyngeal PCR for SARS‑CoV‑2 and multiplex respiratory PCR panels that identify influenza, RSV, and other viruses. Stool PCR is used during norovirus outbreaks to confirm etiology. Viral culture is rare in routine practice and largely reserved for specialized laboratories.
Treatment, Prevention and Public-Health Impact

Treatment and prevention pathways diverge sharply. Antibiotics target bacterial processes; effective antivirals exist for a limited number of viruses and often work best when started early. Vaccination has had major success against many viral diseases and some bacterial ones (for example, pneumococcal conjugate vaccines). Misuse of antibiotics accelerates resistance—an urgent public‑health problem.
Hard numbers put the stakes in perspective: the CDC attributes about 2.8 million antibiotic‑resistant infections and at least 35,000 deaths annually in the United States, and estimates suggest roughly 30% of outpatient antibiotic prescriptions are unnecessary. Those figures drive stewardship programs and vaccination campaigns alike.
7. Treatment differences: antibiotics treat bacteria; antivirals exist for only some viruses and supportive care is common
The fundamental rule is simple: antibiotics work on bacteria and not on viruses. Antiviral drugs exist for select infections—oseltamivir for influenza if started within about 48 hours, and several agents or monoclonals for SARS‑CoV‑2 in specific patient groups and time windows—but most viral illnesses rely on symptomatic care, hydration, and rest.
Empiric IV antibiotics remain lifesaving in suspected bacterial sepsis, whereas routine colds do not need antibiotics. Reducing unnecessary prescriptions protects patients from adverse effects and slows the emergence of resistant organisms; stewardship programs in outpatient and inpatient settings have shown measurable reductions in inappropriate use.
8. Outcomes and public-health impact: vaccination, resistance, and hospitalization burdens differ across bacterial and viral threats
Vaccines have dramatically reduced incidence and severity of many viral illnesses (measles, influenza to varying degrees, COVID‑19 vaccines reducing severe disease) and some bacterial diseases (pneumococcal conjugate vaccine lowering invasive pneumococcal disease in children). By contrast, antibiotic resistance increases hospital length of stay, costs, and mortality, making resistant bacterial outbreaks a priority for infection control.
Public‑health priorities shift accordingly: vaccination campaigns and rapid antiviral deployment for viral epidemics; rigorous infection‑control, antibiotic stewardship, and surveillance for resistant bacterial threats. Examples include pneumococcal vaccination reducing pediatric invasive disease and hospital outbreaks of MRSA or resistant gram‑negatives requiring targeted interventions.
Summary
- Incubation and symptom patterns help clinicians triage: abrupt systemic symptoms often signal viral illness, while focal pain or purulence points toward bacteria.
- Biology matters: bacteria are cellular and culturable; viruses are acellular and usually detected by PCR or antigen tests—this drives diagnostics and treatment choices.
- Antibiotics treat bacterial disease only; antivirals are available for some viruses and work best early. Overprescribing antibiotics fuels resistance (about 2.8 million resistant infections and ≥35,000 deaths yearly in the U.S.).
- Prevention differs: vaccines and nonpharmaceutical measures have outsized effects on viral disease burden, while stewardship and infection control are central to managing bacterial resistance.
Ask your clinician about testing before accepting antibiotics, and keep seasonal vaccinations up to date (influenza, COVID‑19 boosters when recommended) to reduce both individual risk and community spread.