In 1971 President Richard Nixon signed the National Cancer Act, launching what the press dubbed the “War on Cancer.” That declaration focused public attention on research and treatment, but it also fed fear and a rush to definitive answers. Over decades that followed, certainty often gave way to speculation.
The mismatch between scientific nuance and headline-friendly claims has left many people holding on to shortcuts—simple explanations for a complex set of diseases. Those shortcuts can mislead patients, steer prevention efforts off course, and deepen stigma around diagnosis and survival.
Many widely held beliefs about cancer are inaccurate or oversimplified; this article debunks 10 common myths about cancer with evidence, practical examples, and clear takeaways so readers can make better health decisions. Worldwide, cancer caused roughly 10 million deaths in 2020, underscoring why accurate information matters (WHO, American Cancer Society).
Causes and Risk Myths
Misinformation about what causes cancer steers people toward the wrong preventive steps. Strong, consistent evidence links tobacco, certain infections (HPV, hepatitis), alcohol, ultraviolet radiation, and specific occupational exposures to cancer risk. By contrast, only a minority of cancers arise from inherited mutations.
Public-health work—smoking cessation, vaccination, workplace safety—targets the highest-impact causes. For authoritative overviews see the WHO and the CDC. Scientific panels also evaluate suspected environmental links; some have strong backing, others do not (the IARC review process is a useful reference).
1. Myth: Cancer is always hereditary
The idea that cancer must run in the family is common but incorrect. Most cancers are sporadic rather than inherited; estimates suggest roughly 5–10% of cancers are strongly linked to inherited gene mutations.
Hereditary syndromes—like BRCA1/BRCA2 for breast and ovarian cancer or Lynch syndrome for colorectal cancer—are important to recognize because they change screening and prevention choices. Genetic counseling and targeted testing are offered to people with strong family histories, not to everyone (American Cancer Society).
2. Myth: Cell phones and everyday electronics cause cancer
Worries about radiofrequency from phones are widespread. In 2011 IARC classified radiofrequency electromagnetic fields as “possibly carcinogenic to humans” (Group 2B), a cautious label meaning limited evidence and a need for more research.
Since then, large cohort and case-control studies have not shown convincing rises in brain cancer rates tied to typical phone use, and ongoing surveillance has been reassuring. If someone prefers to be extra cautious, using hands-free options or speakerphone reduces exposure without major inconvenience (IARC/WHO).
3. Myth: Artificial sweeteners or specific foods are major cancer causes
Claims that approved artificial sweeteners like aspartame cause widespread cancer in people are not supported by regulatory reviews. Agencies such as the FDA and the EFSA have reviewed the evidence and found no clear link at approved intake levels.
That said, diet does matter: processed red meats and alcohol are established carcinogens (IARC Group 1). Focus on overall dietary patterns—plenty of vegetables, limited processed meats and alcohol—rather than blaming a single sweetener for cancer risk.
4. Myth: Everyday environmental toxins are the main cause of most cancers
Pollution and workplace hazards can cause cancer, but they are not the dominant cause for most people. Tobacco use and infection-related cancers account for a large share of preventable cases worldwide, according to WHO.
Certain occupational exposures do have clear links—classic examples include asbestos and mesothelioma. Public-health measures—smoking bans, vaccination, improved workplace controls—deliver far more population benefit than broad fear of unnamed “toxins.”
Treatment and Survival Misconceptions
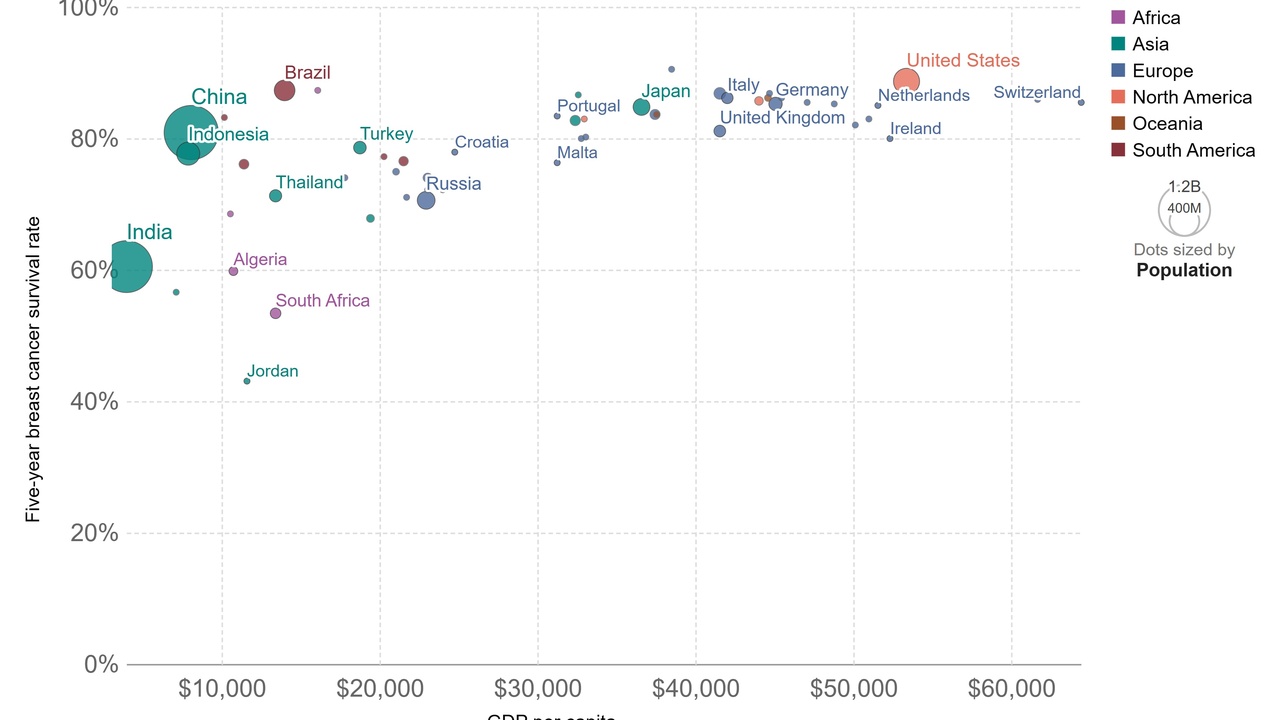
Misconceptions about treatment can steer people away from care that improves survival or quality of life. Modern oncology includes surgery, radiation, chemotherapy, targeted drugs, and immunotherapy, and outcomes have improved steadily since the 1970s.
Registry data show rising 5-year survival for many common cancers in high-income countries, driven by earlier detection and better therapies (SEER, ACS). That progress makes it risky to delay or replace evidence-based care with unproven alternatives.
5. Myth: Chemotherapy causes cancer to spread
Hearing that chemotherapy might “scatter” cancer cells is frightening, but the clinical record is clear: chemotherapy kills rapidly dividing tumor cells and is a cornerstone of curative treatment for many cancers.
Laboratory studies have explored mechanisms that could, in theory, mobilize cells, but those findings do not negate decades of clinical evidence showing adjuvant chemotherapy reduces recurrences and improves survival—for example, in early-stage breast cancer and in curing many cases of testicular cancer. Treatment decisions should rely on oncologists and guideline data.
6. Myth: A cancer diagnosis is a death sentence
That belief comes from older eras, but survival has changed. Overall 5-year survival for many common cancers has risen since the 1970s; localized breast and prostate cancers often have 5-year survival rates above 90% in registries like SEER.
Outcomes still vary widely by type and stage, so staging-specific information matters. Many people now live long lives after cancer, and for several cancers management has shifted toward chronic-care models rather than an automatic fatal trajectory (SEER).
7. Myth: Alternative therapies can cure cancer
The appeal of “natural” cures is understandable, but few alternative treatments hold up to randomized trials. Some historically promoted remedies, like laetrile (amygdalin), have been tested and found ineffective or unsafe.
Choosing unproven therapies in place of standard treatment is associated with worse survival in studies that compare patients who delay or refuse conventional care. Complementary approaches—nutrition support, acupuncture for nausea, mindfulness for distress—can be helpful adjuncts, but they should not replace therapies with proven benefit (NCI).
Social, Screening, and Lifestyle Myths

Misinformation about screening, vaccines, and lifestyle choices affects prevention and follow-up. Accurate understanding of screening trade-offs, the protective power of vaccination, and the benefits of exercise and quitting smoking can change outcomes at the population level.
Screening programs save lives for certain cancers and age groups, but they also produce false positives and overdiagnosis. Vaccines prevent infection-driven cancers, and physical activity improves quality of life and may influence long-term outcomes. Practical, guideline-based decisions beat headlines.
8. Myth: Screening (like mammograms) always saves lives without downsides
Promoting screening comes from a desire to catch cancer early, and in many cases it does reduce mortality. Mammography, for instance, lowers breast cancer deaths in certain age groups while also producing false positives and some overdiagnosis.
Guidelines from bodies like the USPSTF and ACS balance benefits and harms by age and risk. Discuss screening choices with a clinician so decisions reflect personal risk and preferences rather than one-size-fits-all rules.
9. Myth: Cancer patients should rest and avoid exercise
Rest matters, but so does movement. Strong evidence shows that physical activity during and after treatment reduces fatigue, improves function, and boosts quality of life.
Survivorship guidelines often recommend aiming for about 150 minutes per week of moderate activity when safe, adapted to treatment phase and individual capacity. Start low, get team approval, and consider supervised rehab programs when available (ACS).
10. Myth: Vaccines (e.g., HPV) are unsafe or unnecessary because cancer only affects the old
Vaccination skepticism sometimes assumes cancer is only an older person’s problem, but many cancers begin with infections acquired earlier in life. HPV causes about 70% of cervical cancers via types 16 and 18.
Vaccines such as Gardasil markedly reduce HPV infection and precancerous lesions in vaccinated cohorts, with strong safety monitoring backing their use. Harald zur Hausen’s work linking HPV to cervical cancer earned the 2008 Nobel Prize and underpins decades of prevention success (CDC, Nobel Prize).
Summary
- Most people with cancer do not have an inherited syndrome; lifestyle factors, infections, and environmental exposures explain many preventable cases, so focus prevention where it counts (smoking cessation, vaccinations, UV protection).
- Screening and vaccines save lives when used according to guidelines, but screening carries trade-offs (false positives and overdiagnosis), so discuss timing and options with a clinician.
- Evidence-based treatments—surgery, radiation, chemotherapy, targeted therapy, and immunotherapy—have improved survival; delaying or replacing them with unproven alternatives increases risk.
- Practical actions matter: get recommended vaccinations, quit smoking, stay active within medical guidance, and consult trusted sources such as WHO, CDC, or the American Cancer Society when weighing decisions.






